Chronic back pain (CBP), defined as back pain lasting for 3 months or more, is the most common pain condition globally.1 Greater healthcare utilization, productivity limitations and poor quality of life have immediate and long-term impacts on patients and the healthcare system.2 The guidelines recommend physiotherapy as a frontline intervention, alongside education and behavioural interventions.3
For patients living in diverse settings with varied access to healthcare, digital technologies could prove useful in providing a personalized touch and expanding avenues for potential holistic care.
Digital therapies for chronic back pain
A multimodal, 12-week digital care programme for 6,468 patients with CBP, involving disease education, sensor-guided exercise therapy and behavioural health support with personalized virtual health coaching, showed promising results in diverse real-world settings.4 Sixty-eight per cent (4,431 out of a total of 6,468) of patients demonstrated improvement in visual analogue scale pain between baseline and 12 weeks. Some of the available digital technologies have been briefly appraised below.
Mobile health
The path to personalized treatment starts with obtaining more granular data related to diseases in real-life settings from individual patients.5 The data sources could be many and require correlation with physical signs and symptoms. Besides electronic health records, a disease management application (app) or online form reporting outcomes, diurnal variations in symptoms, gender- and age-specific physical activities and mental health status could paint a larger picture of patients presenting with CBP symptoms.
Self-management mobile health (mHealth), comprising educational, physical and psychological interventions, forms the basis of multidisciplinary pain treatment (MPT) programmes. In a meta-analysis of nine studies with 792 participants, Chen et al. showed that disability (mean difference -1.54, 95% confidence interval [CI] -2.35 to -0.73; p<0.001) and pain intensity (mean difference -0.85, 95% CI -1.29 to -0.40; p<0.001) decreased when mHealth and routine care solutions were applied simultaneously compared with usual care alone in patients with CBP.6 Table 1 lists different types of mHealth applications, along with their published evidence of varying degrees of efficacy.7–12
Table 1: Mobile health applications for chronic back pain with published evidence7–12
|
mHealth application |
Key attributes |
Advantages |
Reference |
|
Pain Coach (PainCoach Inc, Nova Scotia, Canada) |
Self-management and assessment, activity tracker and nudges for exercise/behavioural modifications, etc. |
Pain reduction and self-management |
Hogan et al.7 |
|
Well Health (Invitrace Company Ltd, Bankok, Thailand) |
Artificial intelligence and gamification |
Pain reduction and self-management |
Lo et al.8 |
|
selfBack (SelfBACK, Denmark) |
Personalization, education, scheduling and nudges for exercise/behavioural modifications, etc. |
Pain reduction and recovery |
Sandal et al.9 |
|
ACBSC (Not yet available on market) |
Exercise and education |
Self-management |
Mbada et al.10 |
|
PainNavigator (PainNavigator Inc, Chicago, USA) |
Education, target setting, self-management and assessment |
Self-management |
Browne et aI.11 |
|
Kaia (Kaia Health Software GmbH, Munich, Germany) |
Education, scheduling/nudges for exercise/behavioural modifications, etc. |
Pain reduction |
Huber et al.12 |
ACBSC = animated cartoon-based self-care; mHealth = mobile health.
The selfBACK application provides weekly tailored self-management plans, targeting physical activity, strength and flexibility exercises and education for its users.13 The self-management objectives are achieved by creating case-based reasoning to obtain and repurpose insights from earlier successful cases. A single-arm pilot study enrolled 51 patients seeking help (physiotherapy, chiropractic or general practice) for CBP within the past 8 weeks. The primary outcome, disability, was measured using the Roland-Morris Disability Questionnaire (RMDQ).14 This scale assessed low back pain-related self-rated physical disability. At the 6-week follow-up, there was a notable improvement in the RMDQ scores (change in score -1.8, 95% CI -0.7 to -2.9).13 This pilot study was followed by a multinational randomized controlled trial (RCT) with a two-arm design, investigating the effectiveness of the app in a care-seeking CBP population. This study confirmed the utility of the selfBack intervention.9
The Kaia App is an mHealth app adopting a comprehensive evidence-based MPT programme for non-specific low back pain in accordance with current international disease management guidelines.15,16 Efficacy of the app was assessed through an RCT on 101 adult patients. The control group received online education and six physiotherapy sessions over 6 weeks. The intervention group used the Kaia App for 3 months. At the 12-week follow-up, the Kaia App group reported significantly lower pain intensity compared with the control group (2.70 ± 1.51 versus 3.40 ± 1.63, p<0.01), underscoring superiority of the Kaia App compared to physiotherapy and online education.17
Telemedicine
Prescription exercises at home for chronic pain are becoming a viable and cost-effective alternative to reduce healthcare costs. Telemedicine interventions for back pain, such as health education and goal setting, have gained acceptance since the COVID-19 pandemic-enforced restrictions on travel and related logistics.18
Virtual reality
Pain education and cognitive behavioural therapy (CBT) are useful approaches for the management of chronic pain.19,20 Immersive technologies such as virtual reality (VR) could be a potential approach to provide behavioural therapeutics for CBP. One hundred and seventy- nine adults (females: 76.5% and Caucasian: 90.5%) with CBP were enrolled and randomized to two daily VR programmes, EaseVRx (a VR programme with immersive pain relief skills) or a Sham VR (2-dimensional content delivered via a VR headset) for 56 days.21 EaseVRx was superior to Sham VR for all primary outcomes, i.e., change in average pain intensity and pain-related interference with activity, stress, mood and sleep. High rates of engagement and user satisfaction were found with EaseVRx, which could be an effective home-based, on-demand, nonpharmacological treatment for complex CBP.21
Another study termed VARIETY (Virtual reality integrated within physiotherapy for patients with complex chronic low back pain; ClinicalTrials.gov identifier: NCT05701891) is underway to test the utility of integrated physiotherapy with VR for patients with CBP.22,23 In this two-arm study, the cost-effectiveness of physiotherapy with integrated, immersive multimodal (pain education, activation, relaxation and distraction) VR is being compared with the usual primary physiotherapy care. Instead of providing VR as a stand-alone treatment, this pragmatic trial will ensure VR integration by physiotherapists while treating the patients. Multimodal VR interventions can be tailored to individual needs, and hence, provide a personalized approach to treatment. The efficacy and outcomes are expected to be robust due to the thorough monitoring of patients and their treatment, which includes five measurements over a follow-up period of 12 months.22
Conclusion
In conclusion, we emphasize that the aforementioned digital technologies are expected to provide a more data-driven and personalized approach to managing CBP. The evidence for generation and adoption of these technologies is still a work in progress. We anticipate that VR technologies will become mainstream in the coming years and create wide-ranging options for delivering CBT, rehabilitation exercises and remote coaching to patients with CBP virtually, in a more cost-effective and patient-friendly manner. In Figure 1, we have summarized a digital model that outlines a personalized approach for the management of CBP based on short- and long-term data from patients, enabling clinicians to intervene in a customized manner in real-world settings.
Figure 1: Personalized approach to the management of chronic back pain based on short- and long-term patient data from various sources, enabling clinicians to devise customized interventions
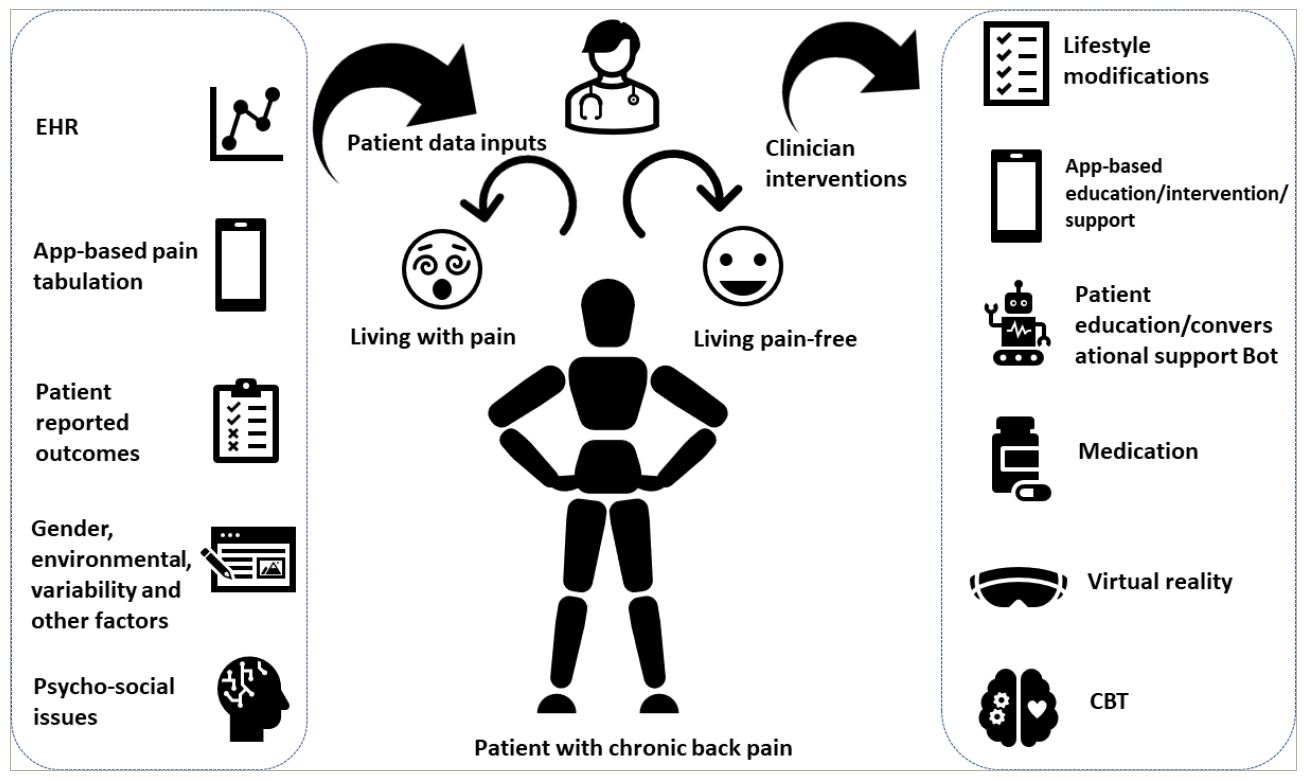
CBT = Cognitive Behavioural Therapy; EHR = Electronic Health Record